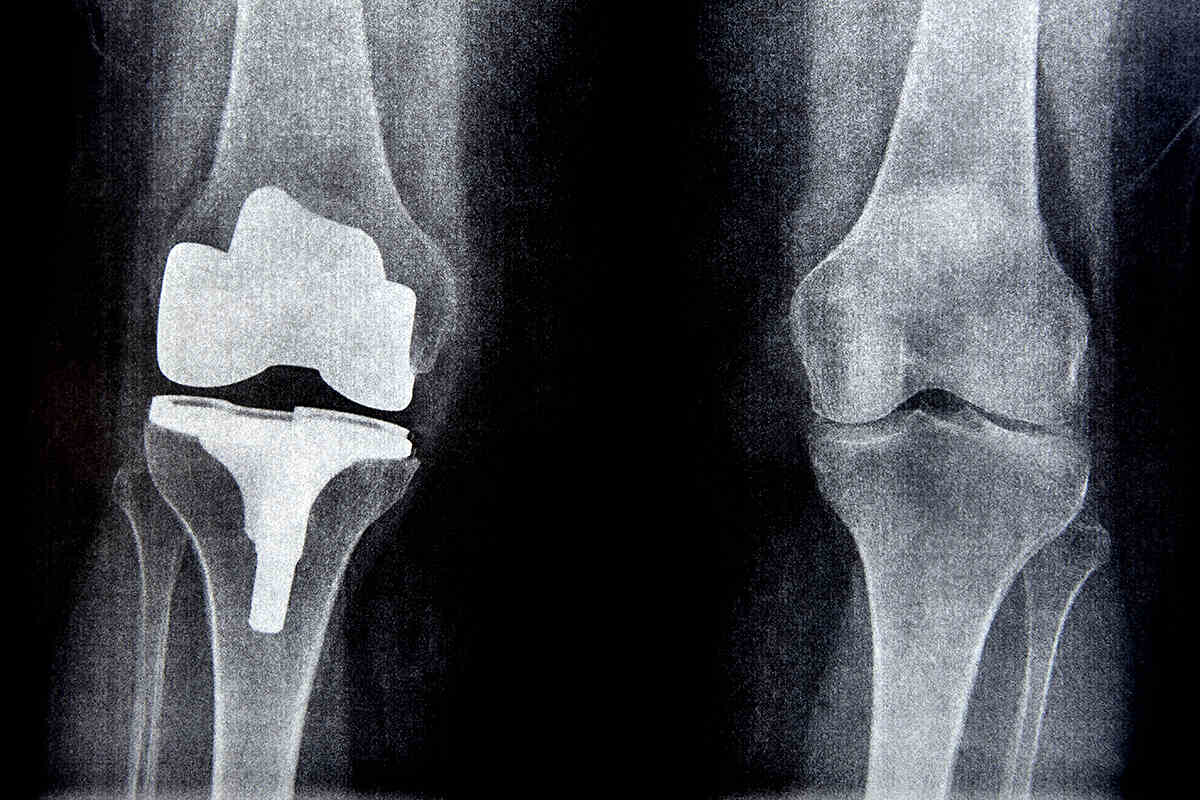
Making the right prosthesis choice, such as a prosthesis for knee replacement, is paramount to your recovery and long-term knee function post-replacement surgery. Our guide clarify the options and steers you through the selection process with consideration for your individual needs.
Key Takeaways
- Knee replacement prostheses are tailored to individual patient needs, influenced by factors like arthritis extent, stability of ligaments, and socioeconomic status, with components designed for stability, resistance, and natural movement.
- Cruciate ligaments are crucial in knee prosthesis design, affecting the decision to retain or sacrifice these ligaments during replacement surgery, which in turn influences knee function, implant stability, and patient satisfaction.
- Advancements in knee prosthesis materials aim to increase durability and compatibility with bone cement, with new materials like titanium alloys and UHMWP enhancing longevity and performance of the implant.
Understanding Knee Replacement Prostheses
A partial knee replacement surgery is fundamentally centered around the prosthesis. These artificial devices are designed to replicate the function of a healthy knee, restoring mobility and relieving knee pain. A typical procedure knee replacement surgery includes the femoral component, tibial component, and patellar component.
Selecting the appropriate knee implant is a significant aspect of the knee replacement process. The choice is influenced by a variety of factors including cost, performance record, and most importantly, the specific needs of the patient. It’s like choosing the right pair of shoes – the right fit is crucial for comfort and functionality.
Types of Knee Implants
When it comes to knee implants, one size does not fit all. From total knee replacements that replace the entire knee joint to partial knee replacements that replace only a portion of the knee, there are various categories to choose from. Each type of implant has its own unique characteristics. For instance:
- Fixed-bearing knee implants have round femoral components that articulate with a relatively flat tibial articular surface.
- Mobile-bearing knee implants offer increased mobility.
- Monobloc and modular knee implants each have their own benefits and drawbacks.
The design of these implants significantly influences their function and lifespan.
Components of a Knee Prosthesis

A knee prosthesis is not a mere piece of metal. It’s a meticulously crafted device made up of several components, each playing a crucial role. The primary constituents of a knee prosthesis include the femoral, tibial, and patellar components, with metal caps crafted from metal alloys such as titanium or cobalt-chromium-based alloys, along with robust plastic parts.
Plastic spacers are another essential part of knee prostheses. They provide stability for the joint and are typically composed of durable plastics, such as medical-grade polyethylene. The design of these components ensures:
- Stability
- Resistance
- Desired motion
- Torque
This facilitates natural knee movement.
Selecting a Knee Implant
Choosing a knee implant requires careful consideration. It’s a decision that is influenced by several factors. For example, the extent of arthritis significantly influences the choice of a knee implant.
Additionally, the stability of the patient’s ligaments is another crucial determining factor. Furthermore, the cost of different implants, the patient’s age, gender, expectations, and socioeconomic status, as well as the overall condition of the hip and knee, also play a significant role in determining the most appropriate implant type.
The Role of Cruciate Ligaments in Knee Prosthesis Design
Your cruciate ligaments, specifically, the anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL), play a pivotal role in knee prosthesis design. These ligaments stabilize the knee joint, prevent antero-posterior displacement of the tibia and femur, and provide rotational stability.
The design of a knee prosthesis is considerably affected by whether these ligaments are present or absent. For instance, retaining the posterior cruciate ligament (PCL) during surgery can enhance the stability and function of the knee prosthesis.
Retaining vs. Sacrificing Cruciate Ligaments
The decision to retain or sacrifice the cruciate ligaments during knee replacement surgery is a complex one. Retaining these ligaments can result in:
- Enhanced knee function, including inherent stability
- Easier ligament balancing
- Reduced stress between bone and cement
- Proprioceptive feedback
- Improved knee flexion
- Overall stable knee movement.
However, retaining the ligaments is not always the best choice. There can be drawbacks such as ligament insufficiency, posterolateral instability, and specific inflammatory conditions that may make it unsuitable for all patients.
On the other hand, sacrificing the ligaments can:
- Ensure better implant stability
- Increase the range of motion
- Enhance knee stability
- Lower the risk of implant loosening
- Potentially increase patient satisfaction
Innovations in Knee Prosthesis Materials
The field of knee prosthesis materials has seen remarkable advancements in recent years. Innovations include:
- Biocompatible materials such as zirconium, titanium alloys, UHMWP (ultra-high molecular weight polyethylene), and smart materials
- Enhancing the longevity of prostheses
- Enhancing wear resistance
- Optimizing compatibility with soft tissues
These advancements focus on improving the overall performance and durability of knee prostheses.
The new materials utilized in knee prostheses provide enhanced durability through their low-friction bearing surfaces and improved wear resistance, thereby contributing to the longevity and stability of the implant. Moreover, assessing the compatibility with bone cement is essential to ensure the long-term stability and fixation of the knee implant, significantly influencing the surgical outcome and the durability of the prosthesis.
Durability of Implant Materials
Considering the durability of knee implant materials is vitally important. The typical lifespan of these materials ranges from 10 to 20 years, with replacements generally required after approximately 15 to 20 years.
Different materials offer varying degrees of durability. For instance, titanium knee implants may offer potential advantages over cobalt-chromium implants, as they are lighter in weight and have a lower modulus, which could indicate differences in durability.
The longevity of knee prostheses can be impacted by various factors such as:
- The type of implant material
- Patient’s age and gender
- Specific diagnosis
- The type of fixation used
- The implant’s design
- Patient selection
- The surgical technique applied
Compatibility with Bone Cement
The compatibility of implant materials with bone cement plays a vital role in the success of knee replacement surgery. Bone cement, particularly polymethylmethacrylate (PMMA) cement, is used to securely adhere the patient’s native bone to the prosthetic components, thereby guaranteeing the stability and reinforcement of the implant.
The materials used in knee prostheses, including titanium- or cobalt-chromium-based alloys for metal components and medical-grade polyethylene for plastic components, are carefully selected to ensure compatibility with bone cement for secure fixation.
Preparing for Total Knee Replacement Surgery
The preparations for total knee replacement surgery hold equal significance as the surgery itself. This includes engaging in preoperative exercise programs, increasing physical activity in daily living, and potentially seeking treatment from a physical therapist.
Certain home and lifestyle modifications are also necessary to ensure a smooth recovery process. This includes:
- Quitting smoking
- Managing dental care
- Adjusting medications as necessary
- Ceasing risky habits
- Starting ‘pre-hab’ exercises
- Maintaining a healthy diet
- Reducing or eliminating medications
- Discontinuing most supplements.
Physical Therapy Considerations
Physical therapy is a key aspect of both preparation and recovery from knee replacement surgery. It involves a series of guided exercises that assist patients in regaining range of motion, enhancing muscle strength, and supporting the healing process.
The suggested duration of physical therapy following knee replacement surgery typically involves an outpatient therapy program lasting between 4 and 8 weeks. This therapy often occurs with a frequency of 3 to 4 times per week for a duration of approximately 3 to 4 weeks. Specific exercises recommended for pre-surgery physical therapy include ankle pumps, thigh squeezes (quadriceps sets), and heel slides.
Home and Lifestyle Adjustments
Home and lifestyle adjustments can greatly aid in recovery after knee replacement surgery. For instance, recliner chairs are recommended as they offer multiple positions and provide comfort and support.
In terms of daily routine, engaging in low-impact activities such as swimming can be beneficial. The recovery period typically spans 6-12 months or more, with full recovery often taking up to a year. It is advisable to rest as needed, while also incorporating regular walking to minimize knee joint stiffness and inflammation.
When it comes to sleeping, the suggested position following knee replacement surgery is on your back.
Post-Surgery Recovery and Care
The recovery process from knee replacement surgery is a long-term commitment. It involves managing pain, preventing blood clots, and navigating rehabilitation. The typical recovery period following knee replacement surgery ranges from 3 to 6 months, with full recovery and optimal benefits from the procedure possibly taking up to a year.
These recommended strategies for reducing the risk of blood clots following knee replacement surgery include:
- Cessation of smoking and weight loss prior to the procedure
- Engaging in exercises to enhance blood circulation
- Wearing compression garments
- Adhering to prescribed blood-thinning medications
- Utilizing intermittent pneumatic compression to support blood return and postoperative circulation.
Managing Pain and Preventing Blood Clots
It is crucial to manage pain and prevent blood clots as part of post-surgery care. Non-pharmacological pain management techniques, such as:
- massage
- acupuncture
- cold packs
- meditation
- relaxation techniques
Certain methods are recommended for managing pain and helping to relieve knee pain after knee replacement surgery.
Physical therapy following knee replacement surgery plays a crucial role in:
- Reducing pain through enhancing functional mobility
- Expanding range of motion
- Building muscle strength
- Reducing swelling
- Preventing scar tissue formation
- Enhancing flexibility and strength of the knee.
Navigating Rehabilitation
The rehabilitation process can pose considerable challenges. The rehabilitation process generally spans approximately 6 weeks for patients to regain their normal daily activities, and it encompasses outpatient therapy that may extend from 4 to 8 weeks.
The standard procedures involve exercises like standing knee bends and incorporation of home exercises into the daily regimen. Patients will progressively elevate their activity levels, often achieving the ability to walk without an assistive device after 3 weeks, with a comprehensive rehabilitation program typically spanning around 12 weeks.
Long-Term Care for Your Knee Replacement
Knee replacement surgery can significantly improve quality of life. However, it also comes with the responsibility of long-term care for your knee replacement. The average longevity of a knee replacement implant is approximately 15 to 20 years.
To prolong the lifespan of your knee implant, engaging in lower impact fitness activities such as:
- golfing
- bicycling
- doubles tennis
- walking
- swimming
can reduce excessive wear on the implant. Walking, stair climbing, cycling, swimming, and low-impact aerobic exercises are recommended for preserving knee replacement functionality in the long term. Regular check-ups, at least once a year, are also advised.
The Impact of Knee Arthritis on Prosthesis Choice
The choice of a knee implant is largely influenced by the type and severity of knee arthritis. In cases of severe arthritis, where non-surgical treatments like exercise therapy and painkillers are insufficient, a total knee replacement may be necessary.
Surgeons must carefully consider a range of factors when selecting a prosthesis for arthritis patients, including improved kinematics, enhanced knee flexion, and proprioception. These considerations are vital for both total and partial knee replacements, particularly if arthritis is confined to a specific area of the knee. Moreover, it is important for surgeons to ensure that patients have a clear understanding of the potential benefits, risks, and alternatives associated with the surgery.
Potential Complications and How to Avoid Them
Despite the potential relief knee replacement surgery can provide, it does carry some potential complications. These can include prosthesis loosening, knee joint stiffness, and the possibility of nerve damage or infection.
However, there are several measures patients can take to mitigate the risk of these complications following knee replacement surgery. These include:
- Early mobilization to prevent blood clots
- Adherence to proper hygiene practices to prevent infection
- Consumption of a balanced diet rich in fiber and fluids
- Gradual escalation of activity levels as advised by healthcare providers
Real-Life Experiences with Knee Prostheses
Gaining insights from real-life experiences can be invaluable in setting expectations for knee replacement surgery. Patients can generally expect to resume many of their regular activities within eight weeks post knee replacement surgery, with a complete recovery typically taking eight to twelve months.
Despite the challenges, the long-term impact of knee replacement surgery is overwhelmingly positive. Knee replacement surgery, particularly total knee arthroplasty (TKA), has been shown to yield a significant level of patient satisfaction and substantial medium- and long-term enhancements in quality of life.
Frequently Asked Questions
What are the three types of knee replacements?
There are four main types of knee replacement surgery.
What is the recovery time for a knee prosthesis?
The recovery time for a knee prosthesis varies depending on the type of procedure. Generally, partial knee replacement recovery takes 3-6 weeks, while total knee replacement recovery takes around 8 weeks. Most patients are 90% recovered after 3 months, but full recovery can take 6 months or longer.
What is the best prosthetic knee?
The best prosthetic knee could include ceramic implants, which are scratch-resistant and have a long life expectancy.
What is the typical lifespan of knee implant materials?
Knee implant materials typically last 10 to 20 years, with replacements usually necessary after 15 to 20 years.